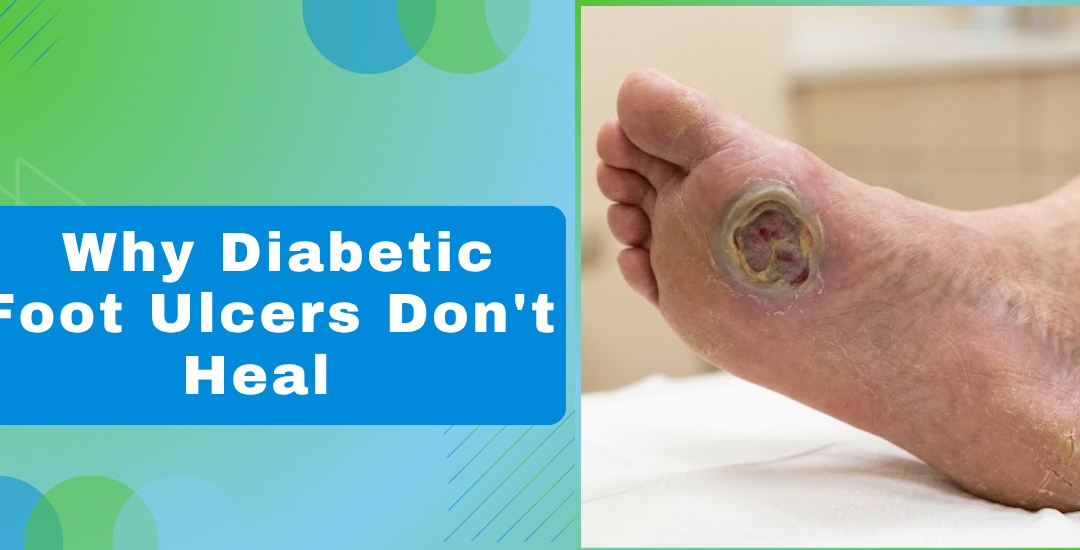
Diabetic foot ulcers don’t heal on their own due to high blood sugar causing poor circulation (peripheral artery disease), nerve damage (neuropathy) that masks injury, and weakened immune responses to infection. Plastic surgeons treat these stubborn wounds through expert debridement, specialized skin grafts, dermal substitutes, and tissue transfer to reconstruct damaged areas and salvage limbs.
|
Why it doesn’t heal |
What a plastic surgeon does |
|
Peripheral artery disease (poor circulation) |
Surgical debridement of dead tissue |
|
Neuropathy (masked injury) |
Specialized skin grafts |
|
Weakened immune response to infection |
Dermal substitutes for wound bed prep |
|
Persistent hyperglycemia stalling repair |
Tissue transfer (flap reconstruction) |
According to Dr. Leena Jain, plastic surgeon in Bandra, A diabetic ulcer that hasn’t closed in four weeks isn’t a wound problem anymore. It’s a circulation and tissue-coverage problem, and that’s where reconstructive surgery changes the outcome.
Why don’t diabetic foot ulcers heal without surgery?
The wound bed in a diabetic foot lacks the basic biology required for closure, oxygen delivery, immune response, and intact nerve signaling. Four mechanisms keep the ulcer open.
Neuropathy: Patients can’t feel the pressure or injury, so they keep walking on it and the wound deepens silently.
Ischemia: Narrowed arteries deliver less blood, and tissue starved of oxygen simply can’t rebuild itself no matter how clean the dressing is.
Infection: Bacteria settle into the warm, sugar-rich wound bed and form biofilms that topical antibiotics can’t reach.
Hyperglycemia: Elevated glucose disables white blood cells, slows collagen formation, and stalls every phase of normal healing.
That’s why standard dressings hit a ceiling. The wound needs structural intervention, not just topical care, and that’s where diabetic ulcer treatment by a reconstructive surgeon becomes the deciding factor between healing and amputation.
What does a plastic surgeon do for a non-healing diabetic ulcer?
Reconstructive plastic surgery treats the diabetic ulcer as a tissue-coverage problem, not a dressing problem. Four interventions, in sequence, restore durable closure.
Debridement: All dead, infected, and biofilm-laden tissue is surgically removed down to a clean, bleeding wound bed.
Skin grafts: A thin sheet of the patient’s own skin is harvested and laid over the prepared wound bed to seal the defect.
Dermal substitutes: Engineered scaffolds are applied to deep wounds where the dermis is missing, giving the body a template to rebuild on.
Tissue transfer: Healthy skin, fat, and sometimes muscle are moved from another part of the body using techniques like perforator flaps to cover exposed bone or tendon.
The reconstructive approach turns a chronic, limb-threatening ulcer into a closed, weight-bearing foot.
Why Choose The Plastic Surgery Clinic?
Dr. Leena Jain is a Plastic, Reconstructive and Microsurgeon with 7+ years of experience, MBBS, MS – General Surgery, and MCh – Plastic Surgery, plus international fellowships in Microsurgery from Hanyang University, Seoul, and Ludwig Maximilian University, Munich. She brings perforator-flap and microvascular expertise directly to limb-salvage cases, and you can read more about her credentials and case work on the Dr. Leena Jain profile.
Her diabetic-foot patients walk again. That’s the metric. Whether the ulcer is on the heel, forefoot, or amputation stump, the focus stays on a closed wound and a foot the patient can stand on.
Wound open longer than a month with no healing?
FAQs
Can a diabetic ulcer heal without surgery?
Small, shallow ulcers with good blood flow can heal with strict offloading and wound care.
How long before a diabetic ulcer needs surgery?
Any ulcer not improving after four weeks of standard treatment needs surgical evaluation.
Does flap surgery prevent amputation?
Yes, well-timed flap reconstruction can salvage limbs that would otherwise need amputation.
Will the ulcer come back after surgery?
Recurrence is possible without offloading, glucose control, and proper footwear after healing.